
Best Night Guards for Teeth Grinding: Reviews & Buying Guide
Do you wake up with a dull headache or a sore jaw that just won’t go away? If so, you are likely part of the

Do you wake up with a dull headache or a sore jaw that just won’t go away? If so, you are likely part of the

Getting a cavity filled is a great first step toward improving your oral health—but what you do afterward is equally important. At Smile Perfection, our

Are you starting to see an open bite or overbite form in your child’s mouth? Are they struggling to pronounce consonant sounds like “D” and
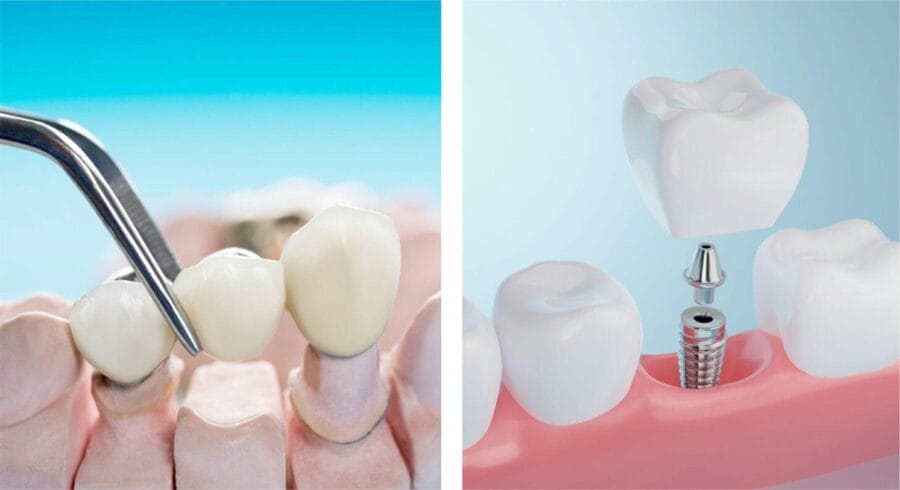
Lost a tooth? It happens. Tooth decay, accidents, and gum disease cause millions to face this situation. The good news is that there are two

If you’re considering a dental bridge or already have one, you’ve probably wondered how long it’ll last you. It’s completely natural to want to know

Every year, millions of Americans hear those dreaded words from their dentist: “You have a cavity.” While cavities are common, ignoring them can lead to
A missing front tooth can shake your confidence and impact daily life in unexpected ways. Modern dentistry offers transformative solutions that restore not just your

Cavities are one of the most common dental issues in children, even with regular brushing and flossing. The good news? Dental sealants offer an easy,

With its scorching heat and dry air, Tucson’s desert climate can have a surprising impact on oral health. From dry mouth to increased sensitivity and

Regular dental cleanings are a vital part of maintaining a healthy smile and preventing oral health problems. Many people may not realize just how much

Dental care is important throughout your life. If you have a filling that is several years old, you may worry about how much longer it

When you get a cavity, you need a filling to prevent further damage to your teeth. But what does a dentist use for tooth fillings?

With so many cosmetic dental procedures available, you no longer have to suffer the embarrassment and insecurity caused by missing teeth. However, it can be

Maintaining a healthy smile helps you look your best. However, improper care for your teeth can result in many issues like cavities and rotting teeth.
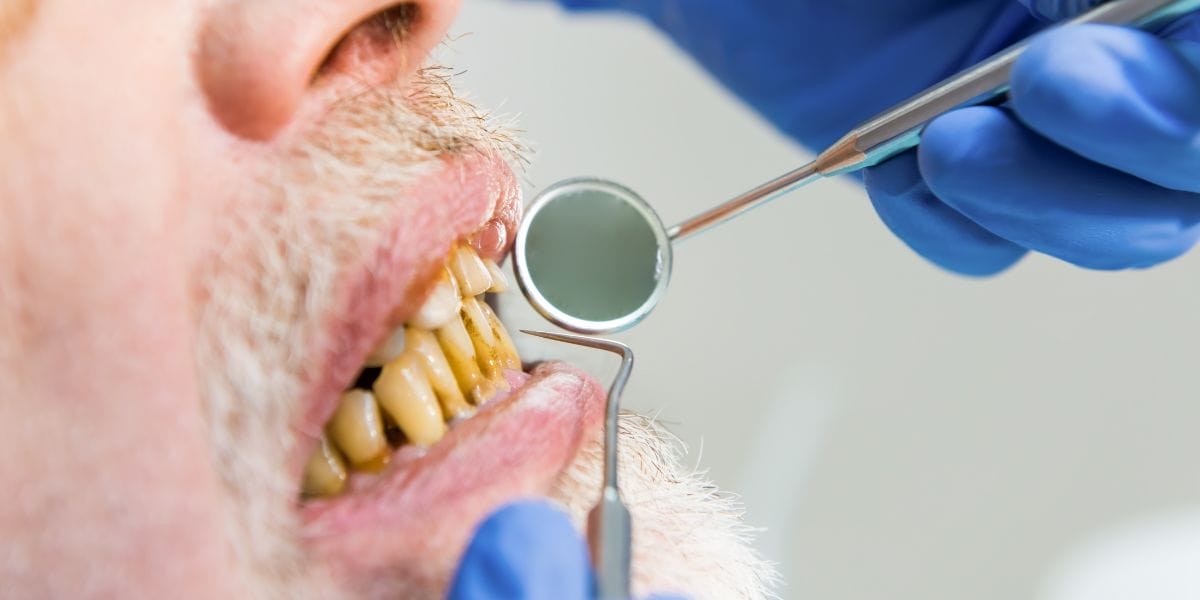
Regular dental hygiene and dentist visits often spare you the dangers of advanced tooth decay. However, if you leave a problematic tooth untreated, you may
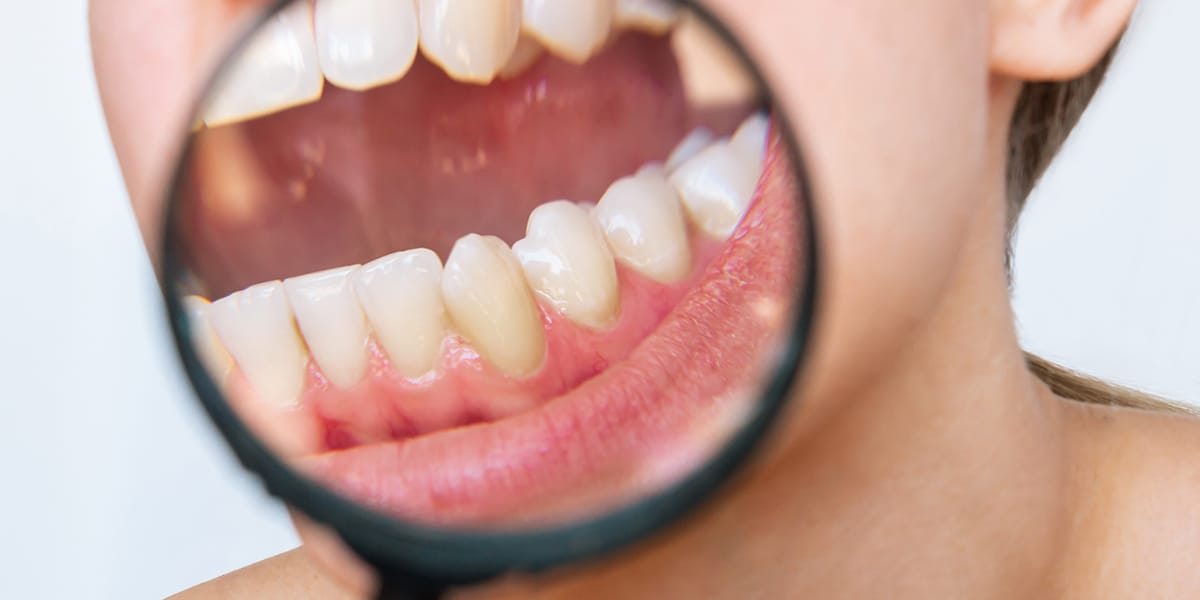
Nobody likes to have bad breath. You can usually easily prevent this unpleasant condition with good oral care. However, many people may adopt faulty oral

Dental care affects much more than your teeth. Bad teeth contribute to physical health problems like gum disease, headaches, and heart disease. You may also
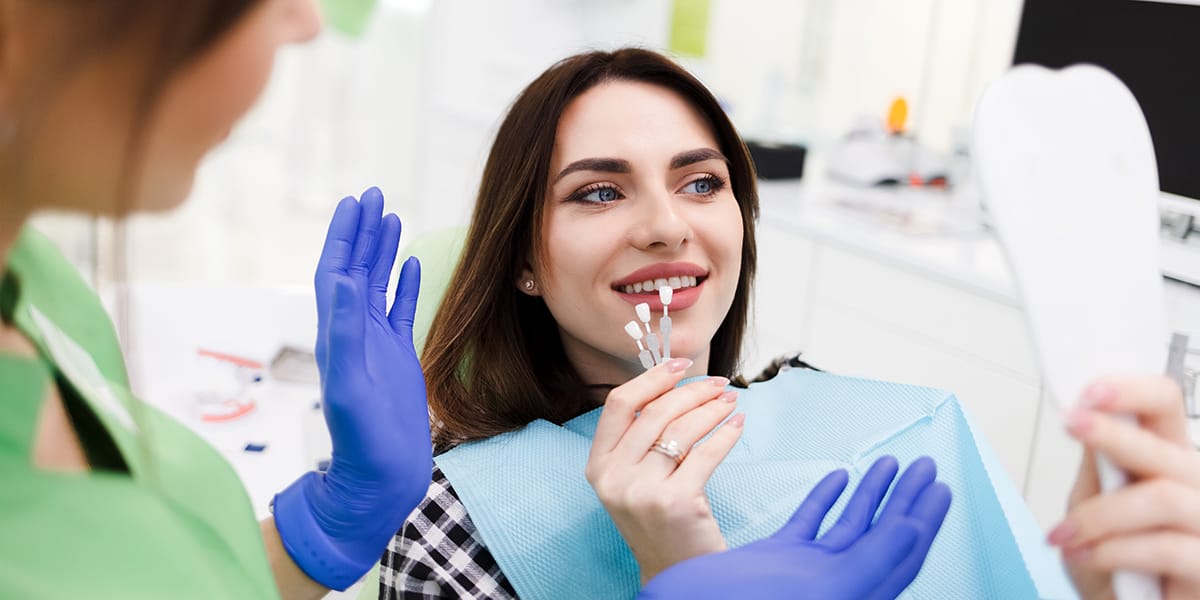
Planning a dental procedure can be stressful, especially if you aren’t sure what procedure you need. In addition, it can be challenging for patients to